Understanding Blood Sugar Support
Blood sugar regulation plays a central role in how the body produces energy, maintains metabolic balance, and supports overall health. Although the concept is often discussed in the context of specific medical conditions, maintaining stable blood sugar levels is a fundamental aspect of daily physiological function for all individuals.
Glucose — commonly referred to as blood sugar — serves as a primary fuel source for cells. After eating, carbohydrates are broken down into glucose and released into the bloodstream, where hormones help regulate how this energy is stored or used. When this regulatory system functions efficiently, energy levels tend to remain stable, supporting cognitive function, physical performance, and overall well-being.
In recent years, interest in “blood sugar support” has expanded beyond clinical discussions into broader wellness conversations. Lifestyle habits, dietary patterns, sleep quality, and stress levels can all influence how the body manages glucose. As a result, many individuals explore strategies aimed at supporting metabolic balance through nutrition, movement, and other evidence-informed approaches.
This guide provides an educational overview of blood sugar support, explaining how regulation works, which factors influence balance, and where nutritional strategies — including supplements — may fit within a broader health context. It is not intended to diagnose, treat, or replace professional medical care but rather to help readers better understand the science behind blood sugar regulation.
Educational Focus of NaturalHealthAtlas
NaturalHealthAtlas develops educational health content focused on explaining metabolic wellness topics through evidence-informed perspectives. Blood sugar support is explored within a broader framework that includes lifestyle factors, nutrition science, physiological mechanisms, and responsible supplement context.
Editorial Scope and Educational Context
This guide is part of NaturalHealthAtlas’ educational content framework focused on explaining health topics within evidence-informed and responsible context. The purpose is to provide clear, science-aligned explanations about blood sugar support, lifestyle influences, and nutritional strategies without promoting medical claims or replacing professional healthcare guidance.
Content is developed using an educational-first approach that emphasizes physiological understanding, balanced perspectives, and contextual interpretation of research rather than promotional messaging. Readers are encouraged to view this resource as a foundational overview designed to support informed learning and critical evaluation of blood sugar support strategies.
How Blood Sugar Regulation Works in the Body
The human body relies on a complex and highly coordinated system to maintain blood sugar levels within a functional range. This process involves hormonal signaling, organ function, and cellular energy needs working together to respond to changing conditions throughout the day.
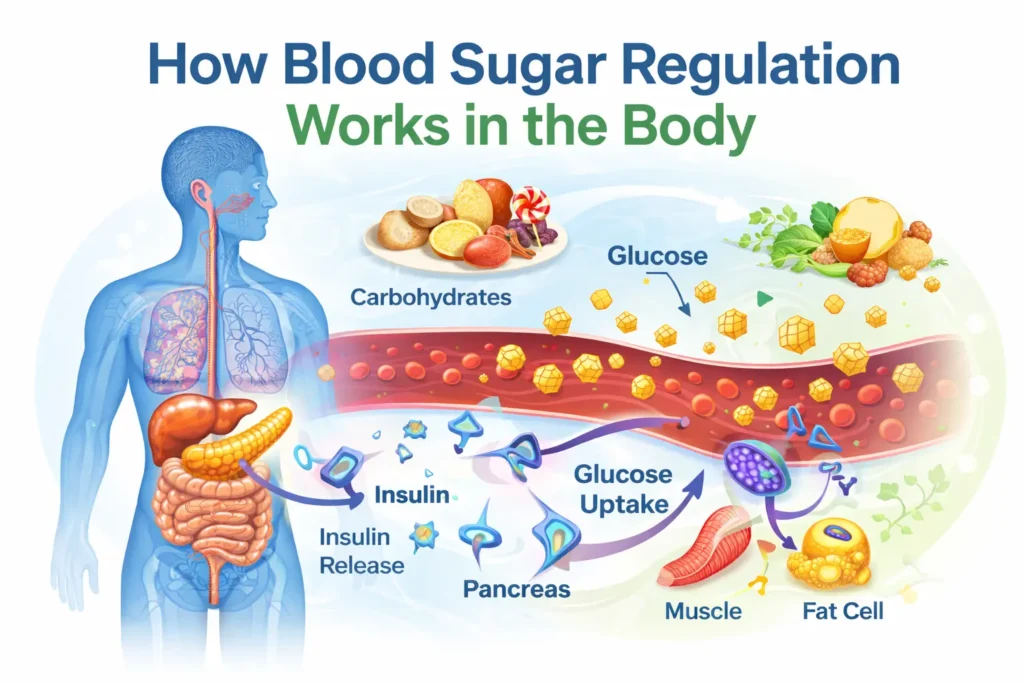
Rather than remaining static, blood glucose levels naturally fluctuate based on factors such as food intake, physical activity, stress, and sleep patterns. The goal of the body’s regulatory mechanisms is not to eliminate these fluctuations entirely, but to maintain balance through dynamic adjustments.
Understanding these biological processes helps explain why lifestyle choices and nutritional strategies can influence metabolic health.
Insulin and Glucose Interaction
Insulin is a hormone produced by the pancreas that plays a central role in blood sugar regulation. After a meal, rising glucose levels signal the release of insulin, which helps transport glucose from the bloodstream into cells where it can be used for energy or stored for later use.
When insulin signaling functions effectively, blood sugar levels tend to rise and fall within a normal physiological range. However, various factors — including dietary patterns, physical inactivity, and metabolic changes over time — may influence how efficiently cells respond to insulin signals.
After a meal, rising glucose levels signal the release of insulin, which helps transport glucose from the bloodstream into cells where it can be used for energy or stored for later use.
Readers seeking a deeper physiological overview may consult educational resources provided by the National Institutes of Health (NIH).
Role of the Liver and Glycogen Storage
The liver acts as a key regulator of blood glucose availability. When glucose levels are elevated, excess energy may be stored as glycogen. During periods of fasting or increased energy demand, the liver can release stored glucose to help maintain stable energy supply.
This buffering role helps prevent extreme fluctuations and supports continuous energy availability between meals.
Cellular Energy Use and Metabolic Signaling
At the cellular level, glucose is used to generate ATP, the molecule that fuels biological processes. Muscle tissue, brain function, and organ systems all rely on this energy production.
Metabolic signaling pathways help determine whether glucose is used immediately or stored. These signals are influenced by hormonal balance, physical activity, and overall nutritional status, highlighting how lifestyle choices can impact blood sugar regulation over time.
Factors That Influence Blood Sugar Balance
Blood sugar regulation is influenced by multiple interconnected factors rather than a single variable. While genetics and underlying health conditions can play a role, daily lifestyle habits often have a significant impact on how efficiently the body manages glucose levels.
Understanding these factors helps provide context for why blood sugar balance may vary from person to person and why sustainable support strategies typically involve a combination of nutritional, behavioral, and physiological considerations.
Dietary Patterns and Carbohydrate Intake
Nutrition is one of the most immediate influences on blood sugar levels. Different types of carbohydrates can affect how quickly glucose enters the bloodstream. Highly refined carbohydrates and sugary foods may lead to faster increases in blood sugar, while fiber-rich foods, whole grains, and balanced meals containing protein and healthy fats tend to support more gradual changes.
Meal timing and portion size can also influence glucose responses. Some individuals may experience greater fluctuations when meals are irregular or heavily concentrated in refined carbohydrates, whereas balanced dietary patterns often promote more stable energy levels throughout the day.
It is important to recognize that dietary responses vary between individuals. Factors such as metabolic health, activity level, and overall nutrient intake can affect how the body responds to similar foods.
Physical Activity and Muscle Function
Movement plays a key role in glucose metabolism. Muscle tissue uses glucose as a primary energy source, and physical activity can help improve how efficiently cells utilize circulating glucose.
Regular exercise — including both aerobic activity and resistance training — may support metabolic flexibility by encouraging glucose uptake independent of insulin signaling pathways. Even light daily movement, such as walking after meals, can influence how the body processes glucose.
Rather than requiring intense training, consistency and sustainability are often more important for long-term metabolic support.
Sleep, Stress, and Hormonal Regulation
Sleep quality and stress levels can significantly influence blood sugar balance through hormonal pathways. Chronic stress may elevate cortisol levels, which can affect glucose regulation and energy utilization.
Similarly, insufficient or disrupted sleep has been associated with changes in insulin sensitivity and appetite-regulating hormones. Over time, these factors may influence eating patterns, energy stability, and overall metabolic health.
Supporting consistent sleep routines and stress management strategies can therefore play a meaningful role in maintaining balanced blood sugar regulation.
Aging and Metabolic Adaptation
As the body ages, natural metabolic changes may influence how efficiently glucose is processed. Changes in muscle mass, hormonal signaling, and physical activity levels can all affect metabolic responsiveness.
These shifts do not necessarily indicate dysfunction, but they may highlight the importance of proactive lifestyle strategies aimed at supporting metabolic resilience over time. Maintaining regular movement, balanced nutrition, and healthy sleep habits becomes increasingly important as metabolic demands evolve.
Signs That Blood Sugar Regulation May Be Challenged
Blood sugar levels naturally fluctuate throughout the day, and occasional changes in energy or appetite are normal. However, some individuals may notice recurring patterns that suggest their body’s glucose regulation could be under increased stress or experiencing reduced efficiency.
It is important to understand that these signs are not diagnostic indicators of any medical condition. Instead, they may reflect general metabolic patterns that encourage individuals to pay closer attention to lifestyle habits, nutrition, and overall health routines.
Energy Fluctuations Throughout the Day
One commonly reported experience is inconsistent energy levels, particularly cycles of feeling energized followed by noticeable fatigue. These fluctuations may occur after meals or during long periods without eating and can sometimes reflect how quickly glucose levels rise and fall.
Stable energy patterns often depend on balanced meals, consistent routines, and effective metabolic signaling.
Increased Cravings, Especially for Sugary Foods
Frequent cravings for sweet or high-carbohydrate foods may be influenced by multiple factors, including sleep quality, stress, and dietary patterns. Rapid changes in blood sugar levels can sometimes contribute to a cycle where energy dips lead to increased desire for quick sources of fuel.
Understanding this pattern can help individuals explore nutritional strategies aimed at promoting more sustained energy.
Fatigue After Meals
Some people report feeling unusually tired or mentally sluggish after eating. While occasional tiredness may simply reflect digestion or meal composition, recurring post-meal fatigue may encourage a closer look at food choices, portion balance, and overall lifestyle factors that influence glucose regulation.
Changes in Concentration or Mental Clarity
Because glucose serves as a primary energy source for the brain, fluctuations in blood sugar may influence cognitive performance for some individuals. Difficulty maintaining focus, temporary “brain fog,” or inconsistent mental energy can sometimes be linked to broader metabolic patterns.
Persistent symptoms, significant fatigue, or ongoing health concerns should always be evaluated by a qualified healthcare professional. This article is intended for educational purposes only and does not provide medical diagnosis or treatment recommendations.
Lifestyle Foundations for Supporting Healthy Blood Sugar
While many discussions around blood sugar focus on specific foods or supplements, long-term metabolic balance is most strongly influenced by daily lifestyle habits. Sustainable routines related to nutrition, movement, sleep, and stress management form the foundation of healthy glucose regulation.

Rather than relying on single solutions, blood sugar support typically involves consistent patterns that help the body maintain stability over time. Small, sustainable adjustments often have a more meaningful impact than short-term or highly restrictive approaches.
Balanced Nutrition Patterns
Nutrition plays a central role in supporting stable blood sugar levels. Meals that combine carbohydrates with protein, fiber, and healthy fats may help promote a more gradual release of glucose into the bloodstream compared to highly refined or sugar-heavy foods consumed alone.
Whole foods such as vegetables, legumes, whole grains, and minimally processed protein sources are commonly associated with balanced energy responses. In addition, paying attention to portion sizes and meal timing may help individuals maintain more consistent energy throughout the day.
Rather than eliminating specific foods entirely, many nutrition approaches focus on balance, variety, and long-term sustainability.
Movement and Muscle Activity
Physical activity helps support how efficiently the body uses glucose. Muscle contractions increase glucose uptake, allowing cells to use circulating energy more effectively. Both structured exercise and regular daily movement contribute to metabolic health.
Resistance training, walking, cycling, and other forms of movement can all play supportive roles. Even light activity, such as short walks after meals, may influence how the body processes glucose.
Consistency tends to be more important than intensity, making sustainable routines a key component of long-term blood sugar support.
Weight Management Context
Body composition and metabolic health are closely connected, although individual needs vary widely. Maintaining a healthy weight range for one’s body can support insulin sensitivity and overall metabolic efficiency.
However, focusing solely on weight may oversimplify the broader picture. Balanced nutrition, physical activity, and healthy lifestyle patterns often provide more meaningful support than short-term dieting strategies.
Sleep and Stress Balance
Sleep quality and stress management play significant roles in hormonal regulation. Chronic stress may influence cortisol levels, while inadequate sleep has been associated with changes in appetite regulation and insulin sensitivity.
Developing consistent sleep routines, managing daily stressors, and prioritizing recovery can help support the body’s natural regulatory systems. These factors are often overlooked but represent important components of long-term metabolic health.
Nutrients and Botanicals Commonly Studied for Blood Sugar Support
In addition to lifestyle strategies, certain nutrients and botanical compounds have been studied for their potential role in supporting healthy glucose metabolism. Research in this area typically focuses on how specific ingredients may influence insulin sensitivity, carbohydrate metabolism, or overall metabolic balance.

It is important to recognize that nutritional supplements are generally considered complementary strategies rather than primary solutions. Individual responses can vary, and scientific evidence ranges from preliminary findings to more established research depending on the ingredient.
The following examples highlight commonly discussed compounds within blood sugar support discussions from an educational perspective.
Chromium
Chromium is a trace mineral involved in carbohydrate and lipid metabolism. Some research suggests that chromium may play a role in enhancing insulin signaling pathways, potentially influencing how the body utilizes glucose.
Dietary sources include whole grains, broccoli, and certain meats, though intake levels may vary depending on dietary patterns.
Berberine
Berberine is a plant-derived compound found in several botanical species. It has been widely studied for its potential metabolic effects, including possible interactions with cellular energy regulation pathways.
Scientific discussions often focus on its role in metabolic signaling, although outcomes may depend on dosage, formulation, and individual context.
Cinnamon Extract
Cinnamon has been explored in nutritional research due to compounds that may influence glucose metabolism. Some studies suggest that certain cinnamon extracts could support insulin sensitivity, though results remain mixed and dependent on preparation type and dosage.
As with many botanical ingredients, quality and standardization can vary between formulations.
Alpha-Lipoic Acid
Alpha-lipoic acid is an antioxidant involved in energy metabolism. It has been studied for potential effects on oxidative stress and metabolic function, which may indirectly relate to glucose regulation.
This compound is naturally produced in small amounts by the body and also obtained through certain foods.
Bitter Melon
Bitter melon is a traditional botanical used in various cultural health practices. Research has explored compounds within the plant that may influence glucose metabolism pathways, although findings remain variable and context-dependent.
Gymnema Sylvestre
Gymnema sylvestre is an herb traditionally used in Ayurvedic practices. Some studies suggest it may influence taste perception related to sweetness and interact with metabolic pathways associated with glucose regulation.
As with other botanicals, scientific understanding continues to evolve.
Where Supplements Fit Within Blood Sugar Support Strategies
Dietary supplements are often discussed within the broader context of blood sugar support, particularly by individuals seeking additional nutritional strategies alongside lifestyle adjustments. While certain ingredients have been studied for their potential role in metabolic health, supplements are generally considered complementary tools rather than primary solutions.
Healthy blood sugar regulation typically begins with foundational factors such as balanced nutrition, regular movement, adequate sleep, and stress management. Supplements may be explored as part of a broader wellness approach, especially when individuals aim to support specific nutritional gaps or metabolic processes.
Because formulations vary widely, evaluating supplements requires careful consideration of ingredient composition, dosage transparency, manufacturing standards, and scientific context. Multi-ingredient formulas may combine several nutrients or botanicals commonly associated with metabolic support, but individual responses can differ based on personal health status, dietary habits, and lifestyle factors.
It is also important to recognize that supplements are not intended to diagnose, treat, or cure medical conditions. For individuals with existing health concerns or those taking medications, professional guidance is essential before introducing new supplementation strategies.
For regulatory context regarding dietary supplements in the United States, readers may review guidance provided by the U.S. Food and Drug Administration (FDA).
As research continues to evolve, many people choose to learn more about how specific ingredients work, potential benefits, safety considerations, and appropriate usage guidance before deciding whether supplementation aligns with their individual needs. Readers interested in a practical example of how a multi-ingredient formula is structured within this context may explore our in-depth Sugar Defender review.
Who May Consider Blood Sugar Support Approaches
Interest in blood sugar support extends beyond individuals managing specific medical conditions. Many adults explore strategies aimed at supporting metabolic balance as part of general wellness, energy management, or long-term health planning.
Rather than focusing on a single profile, blood sugar support approaches may be considered by people experiencing different lifestyle demands, dietary patterns, or age-related metabolic changes. Understanding these contexts can help individuals evaluate whether exploring supportive habits aligns with their personal goals.
Individuals with Sedentary or Low-Activity Lifestyles
Modern routines often involve prolonged sitting, limited movement, and reduced daily physical activity. Because muscle activity plays a role in glucose utilization, individuals with sedentary habits may choose to focus more intentionally on lifestyle practices that support metabolic efficiency.
In these cases, introducing regular movement, improving dietary balance, and exploring broader metabolic support strategies may become areas of interest.
Those Navigating High-Carbohydrate Dietary Patterns
Dietary habits vary widely across cultures and lifestyles. Individuals whose meals frequently include refined carbohydrates or high sugar intake may become more aware of how nutrition influences energy stability and metabolic balance.
Exploring balanced meal composition, fiber intake, and sustainable nutrition patterns often becomes a starting point when considering blood sugar support strategies.
Adults Experiencing Age-Related Metabolic Changes
Natural metabolic shifts can occur with aging, including changes in muscle mass, hormonal signaling, and energy regulation. These changes do not necessarily indicate dysfunction but may encourage a more proactive approach to lifestyle habits that support metabolic resilience.
Many adults begin exploring blood sugar support as part of a broader focus on healthy aging and long-term wellness.
Individuals Seeking Stable Energy and Metabolic Awareness
Some people become interested in blood sugar support simply because they notice patterns in energy fluctuations, concentration levels, or overall daily performance. Learning how nutrition, sleep, movement, and stress influence metabolic balance can help individuals develop more consistent routines.
Safety Considerations and Professional Guidance
While many lifestyle strategies for supporting healthy blood sugar are broadly applicable, individual health needs can vary significantly. Understanding personal context is important when exploring any nutritional or wellness approach, particularly when supplements are involved.
Dietary supplements may interact differently depending on factors such as age, medical history, current medications, and overall metabolic health. For this reason, individuals with existing medical conditions, those taking prescription medications, or anyone experiencing persistent symptoms should seek guidance from a qualified healthcare professional before making significant changes to their routine.
It is also important to recognize that nutritional supplements are not intended to diagnose, treat, cure, or prevent disease. Educational information about ingredients or lifestyle strategies should be viewed as general guidance rather than personalized medical advice.
Choosing evidence-informed approaches, prioritizing balanced lifestyle habits, and consulting with professionals when necessary can help individuals make safer and more informed decisions regarding blood sugar support.
This guide is part of NaturalHealthAtlas’ ongoing educational series on metabolic health and blood sugar regulation.

Exploring Practical Supplement Context
While lifestyle strategies form the foundation of metabolic balance, some readers choose to explore how multi-ingredient formulations are structured within this context. For an educational example of how a metabolic support supplement is positioned, readers may review our in-depth Sugar Defender analysis.
Frequently Asked Questions About Blood Sugar Support
Can supplements lower blood sugar?
Some dietary supplements contain ingredients that have been studied for their potential role in supporting metabolic function or insulin sensitivity. However, supplements are not designed to replace medical treatment or manage diagnosed health conditions independently. Their effects can vary between individuals, and lifestyle factors such as nutrition, movement, and sleep remain foundational for maintaining healthy blood sugar balance.
Is blood sugar support only for people with diabetes?
No. While blood sugar regulation is often discussed in clinical contexts, maintaining stable glucose levels is relevant for general metabolic health. Many individuals explore blood sugar support strategies as part of broader wellness goals, energy management, or healthy aging — even without a diagnosed condition.
Are natural ingredients safe for everyone?
“Natural” does not automatically mean universally safe. Botanical ingredients and nutrients may interact differently depending on personal health status, medications, or dosage levels. Individuals should review ingredient information carefully and consider consulting a healthcare professional before starting new supplementation routines.
How long does it take to notice changes from lifestyle adjustments?
The timeline can vary widely depending on factors such as consistency, individual metabolism, and overall health context. Some people may notice gradual changes in energy stability within weeks, while long-term metabolic adaptations often develop over months of consistent lifestyle habits.
Do lifestyle strategies matter more than supplements?
Lifestyle foundations — including balanced nutrition, regular physical activity, sleep quality, and stress management — are generally considered the primary factors influencing blood sugar regulation. Supplements, when used, are typically viewed as complementary tools rather than standalone solutions.
Building Sustainable Blood Sugar Support: Long-Term Perspective
Supporting healthy blood sugar regulation is best understood as a long-term process rather than a single intervention. The body’s metabolic systems respond to a wide range of influences, including nutrition, movement, sleep patterns, stress management, and overall lifestyle consistency.
Understanding how glucose regulation works provides a foundation for making informed decisions about daily habits and wellness strategies. Rather than focusing on quick solutions, many individuals benefit from gradual, sustainable adjustments that support metabolic balance over time.
Nutritional approaches, physical activity, and recovery practices often form the core of blood sugar support. For some individuals, exploring specific nutrients or supplements may become part of a broader strategy, but these approaches are typically most effective when integrated within a balanced lifestyle context.
As research continues to evolve, maintaining a critical and informed perspective can help individuals navigate the growing number of discussions surrounding metabolic health. Educational resources, professional guidance when needed, and a focus on sustainable habits remain key components of building long-term metabolic resilience.